Dr. Attaman offers prolotherapy treatment at his Bellevue, WA office. Feel free to call our office at 425-247-3359 (Bellevue) or schedule an appointment online, or read on to find out more first. We see patients from all over the US and Canada and beyond.
What is prolotherapy?
Prolotherapy is a regenerative therapy process that allows the body to activate its natural healing processes, often with dramatic and startling results. It involves injecting a solution of medication to damaged tissues to induce low-grade inflammation in the affected area. It is a non-invasive alternative to surgical treatments for a variety of bone, muscle, and joint problems.
This non-surgical procedure relieves chronic pain with an injection that promotes the natural healing of injured tissues and joints. The limited blood supply and poor healing properties of ligaments, cartilage and tendons may make treatment necessary after injury. Prolotherapy is not a treatment for all issues; a careful pre operative consultation is required to determine if a patient will benefit from prolotherapy versus one of many dozens of other treatment options available from Dr. Attaman.
Beware of practitioners (many are not even physicians) who suggest you need 5-20 sessions of prolotherapy; these are universally people with no training in the usage of image guidance, and most have no other tools available to treat you. In general, prolotherapy properly performed under image guidance should require no more than 1-3 treatments.
What Conditions Can Prolotherapy Help with?
Conditions aided by prolotherapy include whiplash, chronic lower back pain, sacroiliac joint pain, joint problems such as chronic tendonitis and sprained ligaments and tendons.
Injecting the Solution
A mixture of concentrated dextrose, glycerin, and low concentration phenol (PDG solution) is injected into and around the injured tissues. PDG is the strongest of the prolotherapy injection solutions in common use. It creates a stronger and more efficacious inflammatory reaction than using dextrose alone. The injection tricks the body into responding as if a new injury has occurred.
This injection is performed by Dr. Attaman using image guidance such as ultrasound or X-ray. This enhances safety, accuracy, and efficacy many times over prolotherapy done without image guidance. It is particularly critical that x-ray image guidance be used for prolotherapy injections performed in the spine; a misplaced needle in the spine may result in nerve injury, paralysis, and even death. Dr. Attaman is one of the few board certified Interventional Pain Management physicians in the country who performs prolotherapy injections in the spine using fluoroscopic X-ray guidance.
Dr. Attaman received extensive training under the late renaissance man Dr. Thomas Dorman, a leader of the “West Coast” school of prolotherapy. This school of prolotherapy was developed by Dr. Milne Ongley after completing his training with the late James Cyriax. This is considered the most advanced and efficacious school of prolotherapy, in which a very detailed biomechanical evaluation is carried out prior to prolotherapy; it is not enough to identify the damaged tissue, rather the entire “kinetic chain” of the patient must be evaluated prior to identifying which structures need to be treated to optimize function. One may think of this as an engineer evaluating problems with a suspension bridge; while only a few cables may be damaged, those few cables can propagate fault along the entire structure. This was labeled as “tensegrity” by architect Buckminster Fuller.
The second vital component to the “West Coast” school of prolotherapy is the integration of manual therapy into the Prolotherapy session prior to injection. As a board certified Osteopathic Physician, Dr. Attaman applies hands on Osteopathic Manipulative Medicine of the structures in poor alignment immediately prior to Prolotherapy. This is particularly important when performing Prolotherapy in the spine to ensure normal “alignment” prior to injection.
This detailed pre-operative biomechanical assessment of the patient’s kinetic chain and pre-operative manipulative medicine is unique to the “West Coast” school of Prolotherapy and not an integral part of the form of Prolotherapy taught by Drs. Hemwall and Hackett. It is Dr. Attaman’s experience that the “West Coast” school of prolotherapy is much more efficacious.
How Prolotherapy Works
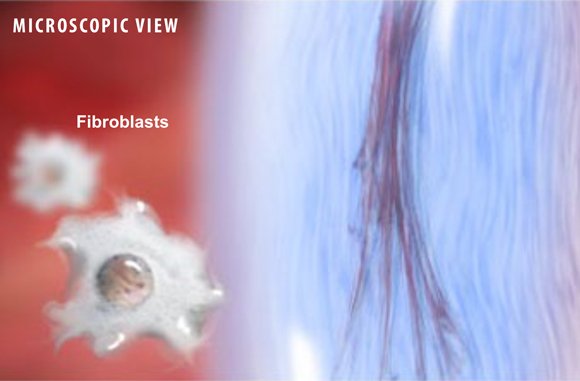
This attracts cells that specialize in repairing damaged tissue. These cells include fibroblasts, which create the collagen used to strengthen and rebuild any damaged tissue.
Long-term Outcome
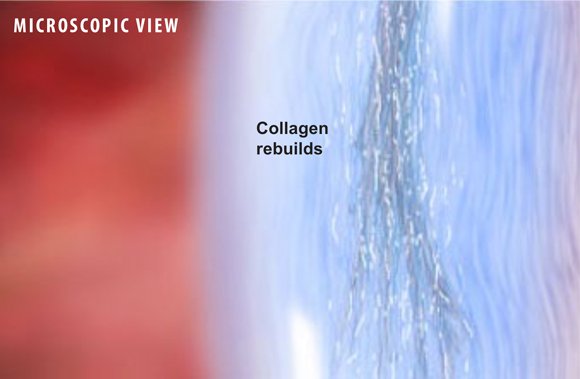
Prolotherapy patients are able to go home the same day, and should avoid taking any anti-inflammatory pain medications (aspirin, ibuprofen and naproxen). Full recovery from inflammation usually occurs within one week of the procedure. Additional treatments may be required to ensure complete healing of the injured tissues.
A Way to Ensure Long-Term Pain Relief and Real Injury Repair
If you’ve got severe joint problems, repetitive stress injuries, or old injuries that flare up and cause you pain, you might consider prolotherapy performed by Board Certified pain-management physician Dr. Jason Attaman. Often it is an effective treatment option for certain bone, muscle, and joint problems.
Our office is in Bellevue, WA, and we have helped patients from all over the US and Canada (with many Canadian patients coming from British Columbia). I may be able to help you, too.
You can contact my office today if you’re interested in prolotherapy, or you can read on to find out more.
Isn’t inflammation a bad thing? Why would you induce inflammation on purpose?
Inflammation is a natural part of your body’s healing processes. When you are injured, your body uses inflammation to increase the flow of growth factors to the affected area.
The problem is that when we’re injured, we tend to reach for ibuprofen, aspirin, or NSAIDs to deal with the pain and to reduce the swelling. That means growth factor levels decrease, and healing tends to remain incomplete.
Prolotherapy allows us to “jump-start” this healing process, restarting it in a safe and effective way. There’s also no need to take over-the-counter painkillers that might interfere with the process. We add a non-interfering painkiller to the injection in order to manage any discomfort. The inflammation we produce is low-grade, mild inflammation, and so you won’t experience the kind of extreme swelling that you might experience directly after suffering an injury.
Is prolotherapy safe?
Yes. Most people experience very few side-effects, if any. Sometimes there is bruising or tenderness at the injection site. Some patients experience adverse reactions to the medication in their injection, and there are a few other risk-factors, which you should discuss with your prolotherapy physician.
We are one of the only clinics in Washington to perform prolotherapy under image guidance using ultrasound and x-ray. This makes the treatment much safer and effective.
What kinds of injuries does prolotherapy treat?
Prolotherapy can mitigate many kinds of musculoskeletal and joint problems. These include tendonitis, arthritis, back pain, sprains and tears, degenerative disc or joint diseases, knee injuries, carpal tunnel disorder, sciatica, sports injuries, whiplash, and more.
Prolotherapy has few side-effects, is minimially-invasive, and can serve as an alternative to surgery in some cases. Furthermore, prolotherapy usually creates significant long-term improvements, to the point where additional treatments may become unnecessary. For many patients, the pain simply disappears once the treatment is complete.
Is prolotherapy considered to be an “alternative therapy?”
Though prolotherapy is not widely practiced, it nevertheless has been a known and reputable technique in Western medicine since 1939. Recent research has rendered the therapy more effective than ever.
Prolotherapy is practiced by medical doctors all over the country. If you’re interested in an in-depth look at the therapy and what it has to offer, take a look at this 2011 medical white paper.
The American Association of Orthopedic Medicine also recognizes prolotherapy as a valid and effective treatment.
Prolotherapy has even been featured in The New York Times.
So why haven’t you heard more about prolotherapy? Some physicians may have trouble believing that treating these issues can be so simple and inexpensive. Any time we speak of “activating the body’s natural ability to heal,” some doctors grow skeptical. When prolotherapy receives recognition, often it’s a grudging recognition. It’s also not as profitable as some other methods of treatment, which may concern some medical and pharmaceutical actors.
Does prolotherapy hurt?
Everyone is different, but prolotherapy can hurt a little bit. You are getting a shot, after all. Our office provides pain-management aids when we perform prolotherapy, however. First, we numb your skin with strong numbing medications. Then, we numb the damaged tissues that need Prolotherapy treatment. Next, we inject the prolotherapy medication. Most people say it feels like getting a vaccination or some blood drawn.
Of course, any pain or discomfort associated with prolotherapy can’t compare to the pain and long-term impacts of surgery, or the long-term pain and effects of simply leaving your condition untreated.
How much does prolotherapy cost?
When you come to our offices we’ll present you with a comprehensive and personalized treatment plan. We’ll include pricing so you’ll know exactly what to expect. The average patient needs one to two shots to experience relief. Some patients will get all of the benefits of prolotherapy that they need after just 1 injection. Everyone is different.
Is prolotherapy covered by health insurance?
No. But your insurance company may also not cover surgery – especially elective surgery – if surgery even is a solution to your pain. Surgery itself can take a toll on your well-being. The question is whether you’d like to try a relatively inexpensive possible solution that maximizes your body’s natural healing system before trying more-expensive, more-invasive procedures.


My husband is a c8 quad he was injured in 1983 for the last 5 years or more he has had terrible low back pain radiating into his hips he has had several injections and they do help but not complete pain relief and only for a short time He also has hip arthiritis on both sides but pain only on left side and more on the lower left side of back Do you think there is anything that will help his pain Thank you Janine Roberts
Dear Janine,
This is too complex to answer over the internet. I’d suggest scheduling a consultation. Best of luck, Dr. Attaman
Hello,
I’m wondering if your practice is strictly for treating an already diagnosed injury, or do you assist in diagnosis? Based on what Dr. Google has told me :) I believe I have ischial bursitis, or possibly some other injury to the ischial tuberosity. I’m seeing my PCP in a few weeks but thinking they are not experts in this and will probably either send me right for physical therapy or to someone else for diagnosis of exactly why I have a lot of pain in my sitz bone (both sides, but worse in one) when sitting for any length of time. So basically I’m just trying to set myself up for the next step. Thank you.
Absolutely, I make diagnoses all the time on every patient I see, that is what makes a physician a physician!
I cannot answer this unless I evaluate you in clinic or review your records. I’d be happy to see you in my clinic and review your MRIs and perform a physical exam. I can also evaluate you via a video conference here:
https://intakeq.com/booking/OmXdxU
Kind Regards, Dr. Attaman
I have just been diagnosed with CPPD (chondrocalcinosis) in my right knee. There is a possibility that the same condition may be affecting the joints in my feet.
Does prolotherapy help with this condition?
My doctor is suggesting I do cortisol injections to relieve the pain and stiffness, and I am leary of cortisol.
I’m wondering if you also utilize autologous PRP in place of the traditional prolotherapy mixture. If not, will you offer your thoughts regarding why? Thanks,
Thank you for sharing this informative article on prolotherapy treatment. It’s great to know that there are non-surgical options available to relieve chronic pain and promote natural healing of injured tissues and joints. It’s also reassuring to hear about the careful pre-operative consultation required to determine if a patient will benefit from prolotherapy, and to beware of practitioners who suggest unnecessary sessions. Dr. Attaman’s use of image guidance for prolotherapy injections is impressive and highlights the importance of safety and accuracy in the procedure. The integration of manual therapy prior to injection as part of the “West Coast” school of prolotherapy is also intriguing and shows a dedication to optimizing function and overall biomechanical assessment. Overall, this article is a great resource for anyone considering prolotherapy treatment and seeking a qualified practitioner like Dr. Attaman.